The Centers for Medicare & Medicaid Services (CMS) have been monitoring therapy utilization trends over the past decade. This month CMS issued its most recent memorandum regarding trends in ultrahigh therapy utilization. The information in this newsletter is to inform skilled nursing facilities (SNFs) of the government's continued scrutiny related to therapy utilization and to provide SNFs with guidance for internally monitoring therapy utilization rates.
CMS-Observation in Therapy Utilization
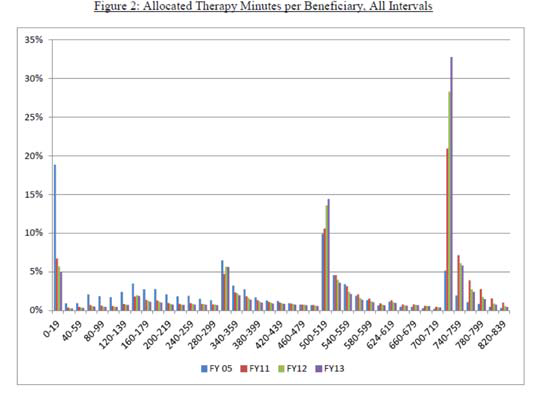
Between fiscal year (FY) 2011 and FY 2012 the rate for utilization of the ultar-high resource utilization group (RUG) increased 4%, whilie all other therpay RUG categories remained teh same or showed a decrease in utilization. In FY 2013 the utilization of ultra-high therapy continued to steadily increase. The second trend identified by CMS wateh concentration of therapy minutes provided at the threshold to qualify for the particular RUG category. This trend was particularly prevalent with RU and RV categories, which accounted for 75% of therapy RUG utilization in FY 2013. This clustering or "grouping" of therapy minutes around the minimum minute required cutoff applied to only 5% of ultra-high therapy RUGs in FY 2005 and has since increased to 33% in FY 2013. The chart below illustrates the incidence of therapy grouping between FY 2005 and FY 2013.
Medicare Payment Advisory Commission (MedPAC)
MedPAC provided comments regarding the increase of Medicare payment rates for SNFs in response to CMS' proposed rule regarding the prospective payment system (PPS) for FY 2015 issued on May 6, 2014. MedPAC stated that no update to the payement rates were deemed necessary, considering that the aggregate Medicare margin for freestanding SNFs in FY 2012 was 13.8%, marking the thirteenth consecutive year exceeding 10%.
MedPAC also noted that trend of therapy days increasingly being classified into ultra-high RUGs are consistent with payment-driven patterns of care and not based on resident need. MedPAC cited that a study conducted by the Office of Inspector General (OIG) concluded that the changes to the resident population treated in SNFs did not explain the intesification in therapy services provided. Furthermore, MedPAC also noted the high incidence of providing residents with just enough therapy minutes to qualify for the highest reimbursing therapy RUGs.
Consequently, MedPAC is urging CMS to revise the PPs system and reconsider any update the Medicare payment rates for FY 2015.
Guidance for SNFs
1. Faciliites should assess how much therapy is being provided with emphasis on the provision of ultra-high therapy levels through the use of routine audits.
2. Validate that the outcomes, intensity of therapy, and the duration of the therapy services are appropriate forthe episode of care.
3. Facilities should also review records for the residents who have high scores for assistance with acitivites of daily living (ADLs).
4. Verify that the medical record supports the level of assistance and support as coded on the MDS.
5. Establish open communication between SNF and therapy company. Focus on providing resident centered care.